What is the Sciatic Nerve?
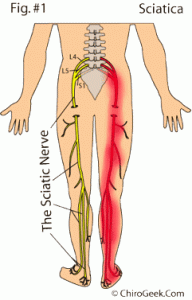
The Sciatic nerve is the main nerve traveling down the leg. This nerve starts in the spine and runs down the back of each leg. This nerve controls the muscles of the back of the knee and lower leg and provides sensation to the back of the thigh, part of the lower leg, and the sole of the foot.
What Is Sciatica?
Sciatica is pain associated with the sciatic nerve which usually originates higher along the spinal cord when nerve roots become compressed or damaged from narrowing of the vertebral column or from a slipped disk. Symptoms can include tingling, numbness, or pain, which radiates to the buttocks, legs and feet.
Common causes of Sciatica include:
- Piriformis syndrome (The piriformis muscle, located in the buttocks, irritates the Sciatic nerve)
- Slipped Disc, Herniated Disc, Bulged Disc
- Degenerative Disc Disease
- Spinal Stenosis, narrowing of the canal
- Pelvic injury or fracture
What Does Sciatica Feel Like? How Do I Know If I Have Sciatica?
Sciatic pain can vary widely. It may feel like a mild tingling, dull ache, or a burning sensation. Some patients describe it as a “hot poker” or a shooting electrical pain. In some cases, the pain is severe enough to make a person unable to move.
The pain most often occurs on one side. Some people have sharp pain in one part of the leg or hip and numbness in other parts. The sensations may also be felt on the back of the calf or on the sole of the foot. The affected leg may feel weak.
The pain often starts slowly. Sciatic pain may get worse:
- After standing or sitting
- At night
- When sneezing, coughing, or laughing
- When bending backwards or walking more than a few yards, especially if caused by spinal stenosis
What Are the Main Symptoms of Sciatica?
- Pain. It’s especially likely to occur along a path from your low back to your buttocks and the back of your thigh and calf.
- Numbness or muscle weakness along the nerve pathway in your leg or foot. In some cases, you may have pain in one part of your leg and numbness in another.
- Tingling or a “pins-and-needles” feeling, often in your toes or part of your foot.
- A loss of bladder or bowel control. This is a sign of Cauda Equina syndrome, a rare but serious condition that requires emergency care. If you experience loss of bladder or bowel control, seek medical help immediately.
Although most people recover fully from sciatica, it can potentially cause permanent nerve damage. Depending on what’s causing the nerve to be compressed, other complications may occur, including:
- Loss of feeling in the affected leg
- Loss of movement in the affected leg
- Loss of bowel or bladder function
© 1998-2010 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. A single copy of these materials may be reprinted for noncommercial personal use only. “Mayo,” “Mayo Clinic,” “MayoClinic.com,” “EmbodyHealth,” “Enhance your life,” and the triple-shield Mayo Clinic logo are trademarks of Mayo Foundation for Medical Education and Research.
References
Clarke JA, van Tulder MW, Blomberg SE, et al. Traction for low-back pain with or without sciatica. Cochrane Database Syst Rev. 2007;(2):CD003010.
Chou R, Qaseem A, et al. Diagnosis and treatment of low back pain: a joint clinical practice guideline from the American College of Physicians and the American Pain Society. Ann Intern Med. 2007;147(7):478-491.
How Does Spinal Decompression Work?
Non-Surgical Spinal Decompression, not to be confused with linear traction, slowly lengthens and decompresses the spine, creating negative pressures within the discs.This reversal of pressure creates an intradiscal vacuum that helps to reposition bulging discs and pull extruded disc material back into place, taking pressure off pinched nerves. Spinal experts believe that nutrients, oxygen, and fluids are drawn into the disc to create a revitalized environment conducive to healing.
What are the Treatments Like?
At the beginning of each session, you will be comfortably fitted with a harness designed to achieve optimal decompression of the low back or neck. During a session of spinal decompression, you will notice a slow lengthening of your spine as your discs are gradually decompressed and relieved of pressure. The treatment process is safe and relaxing. While some patients with extensively injured discs have reported mild discomfort during the first few treatment sessions, their discomfort subsides upon subsequent visits. A patient safety switch provides an extra safety feature, allowing you to stop at any point should you feel discomfort. Each treatment session lasts approximately 30 minutes. Individual patient results may vary.
What is the Typical Treatment Protocol?
A typical spinal decompression treatment protocol consists of about 20-25 sessions over four to six weeks. Some conditions require fewer visits; some require more. Many patients report relief from their pain and other symptoms during the first few treatment sessions, and most experience dramatic pain relief after completion of their prescribed treatment program.
Why Is Spinal Decompression Different from Traction? Why are Some Spinal Decompression Tables Better Than Others?
While traction, physical therapy, and manipulation may reduce disc pressures to as low as 40 mm Hg, only spinal decompression has been shown to achieve negative pressures within the spine. It has been clinically proven that spinal decompression creates negative pressures as low as -110 mm Hg3 within the injured disc during the treatment session. Normally, pulls exerted on the spine trigger sensory receptors in the back to tighten the muscles surrounding the vertebrae and discs in an effort to protect them from injury,a mechanism in the body known as the proprioceptor response. Spinal Decompression bypasses this response by slowly pulling on the spine and relaxing the back over an extended period of time, allowing the spine to be repositioned without tension and without setting off the “Iock down” proprioceptor response. It is important for patients to make sure that they are treated on a high quality spinal decompression table and not an imitation spinal decompression table.
If you have more questions please go to the Frequently Asked Questions Section (FAQ’s) or call us anytime.
How do I Know if I Qualify for Care?
During the complimentary consultation the doctor will ask you questions about your condition such as “Where does it hurt? What makes the pain better? What makes it worse? How bad is it and what else have you tried that hasn’t worked.” Then the doctor will perform a thorough examination and review any x-rays or MRI reports. At this point the Doctor will determine if you are a candidate for our program. If you don’t qualify for the program we can refer you to someone who may be better able to help.
If you are accepted into the program the doctor will make his recommendations on which therapies will help your condition the most and how frequently you will need to come. Most patients will respond to care between 7 to 15 treatments. Some patients may need less, some may need more. Call us today to see if you qualify!
Call Us At:

